If you’re reading this, you’ve probably already been through a lot. Maybe you’ve spent months, or even years trying to conceive. Maybe a doctor recently sat across from you and said words like “diminished ovarian reserve” or “poor egg quality,” and the world felt like it tilted. Maybe you’re just beginning to explore what’s possible, and someone mentioned donor eggs, and now you’re here, wondering what it all means.
Whatever brought you to this page, we want to say something first: you haven’t failed. You are doing something extraordinary – you are finding a new way.
IVF with donor eggs is one of the most effective fertility treatments available today, with live birth rates that can be 40–55% per cycle that remain remarkably consistent regardless of the recipient’s age. Hundreds of thousands of families around the world have been built this way. And yet, almost no one talks about what the journey actually feels like, what every medical step actually involves, or what happens when things don’t go to plan.
This guide is our attempt to change that.
We’ve written this for complete beginners. We’ll walk you through every step of the process in plain language, give you the real data on success rates (not just the marketing-friendly headlines), help you understand what donor selection actually involves, explain the costs honestly, and, importantly, make space for the emotional experience that runs underneath all of it.
There is a lot to take in. Take your time with it.
Why People Choose Donor Eggs and Why the Decision Can Feel Overwhelming
Common reasons intended parents turn to donor eggs
Donor egg IVF is recommended when a person’s own eggs cannot be used, or are very unlikely to result in a healthy pregnancy.
The most common reasons include:
Diminished ovarian reserve (DOR): The ovaries contain fewer eggs than expected for someone’s age. This is detected through blood tests measuring AMH (anti-Müllerian hormone) and FSH (follicle-stimulating hormone), and through an antral follicle count via ultrasound.
Premature ovarian insufficiency (POI) or premature ovarian failure (POF): The ovaries stop functioning normally before the age of 40. This may be spontaneous, genetic (Turner syndrome, Fragile X), or caused by medical treatment such as chemotherapy or radiation.
Advanced maternal age: Egg quality naturally changes with age, particularly after 38–40. For some women in their mid-40s, the chances of a successful pregnancy using their own eggs become quite limited, and this is where donor eggs can make a profound difference. Using eggs from a young, screened donor can restore live birth rates to 40–55% per transfer, regardless of the recipient’s age. The uterus remains capable of a healthy pregnancy well into the mid-50s; it is egg quality, not the ability to carry a pregnancy, that changes with time.
Repeated IVF failure: Some people have undergone multiple rounds of IVF with their own eggs without success. When poor embryo quality is identified as the consistent limiting factor, donor eggs offer a meaningful change in outcome.
Genetic conditions: If one or both partners carry a serious genetic disorder, such as Huntington’s disease, BRCA1/BRCA2 mutations, or other inheritable conditions, using donor eggs (combined with preimplantation genetic testing if needed) could reduce the risk of passing it on.
Absent or inaccessible ovaries: Surgical removal of the ovaries, congenital absence, or other anatomical conditions.
You may fall into one of these categories, or you may have a combination of factors. Your fertility specialist will have explained why they’re recommending donor eggs. If you’re unsure, it’s always okay to ask them to explain again – there are no foolish questions here.

The grief nobody talks about
Here’s something that almost no clinic brochure will tell you: deciding to use donor eggs often arrives with grief. Real, significant grief. And that’s completely normal.
Even when the logical part of your brain understands it’s the right path forward, many people describe mourning the genetic child they’d imagined. That grief doesn’t mean you’re making the wrong choice. It means you are human and you had hopes.
In an informal community poll run with Donor Egg Bank USA, 100% of respondents said they had experienced infertility grief, 62% worried about feeling like a “real” parent, and 79% had concerns about how others would perceive their family. These numbers come from a self-selected online community rather than a formal study, but if you’ve felt any of these things, you are very clearly not alone.
These fears are incredibly common, and, as we’ll discuss later in this guide, the research on family outcomes after donor egg IVF is powerfully reassuring. Most parents describe bonding with their children as immediate, fierce, and indistinguishable from what they’d imagined.
But first: if you’re grieving right now, you don’t have to rush past that. Acknowledging it, talking to a therapist who specializes in fertility, or connecting with communities of other parents who’ve been through this can make an enormous difference. We’ll share some specific resources at the end of this guide.
A decision framework: comparing your options
If you’re in the early stages of exploring, it may help to see donor egg IVF in the context of other paths. Here’s an honest comparison:
Continuing with own-egg IVF: If your specialist has recommended donor eggs, it’s usually because the data on your own eggs isn’t in your favor. More cycles with poor-quality eggs carry significant emotional, physical, and financial costs. That said, some people choose to try one or two more own-egg cycles before moving to donor eggs, and that’s a valid personal choice. Have an honest conversation with your doctor about your individual prognosis.
Embryo donation (also called embryo adoption): Instead of using a donor’s fresh or frozen eggs, you receive an embryo that was created by another couple during their IVF treatment and later donated. This is less expensive than donor egg IVF and follows a very similar process (endometrial preparation and transfer), but you have less control over the genetic profile of the embryo, and the selection process differs significantly.
Adoption: A separate path entirely – emotionally, legally, and practically. Some families pursue both simultaneously; others choose one or the other. Adoption timelines and availability vary enormously by country.
Remaining child-free: A legitimate choice, and one that deserves acknowledgment rather than pressure. If you’re not ready to decide, that’s okay too.
This guide focuses specifically on donor egg IVF, so let’s get into the details of how it works.
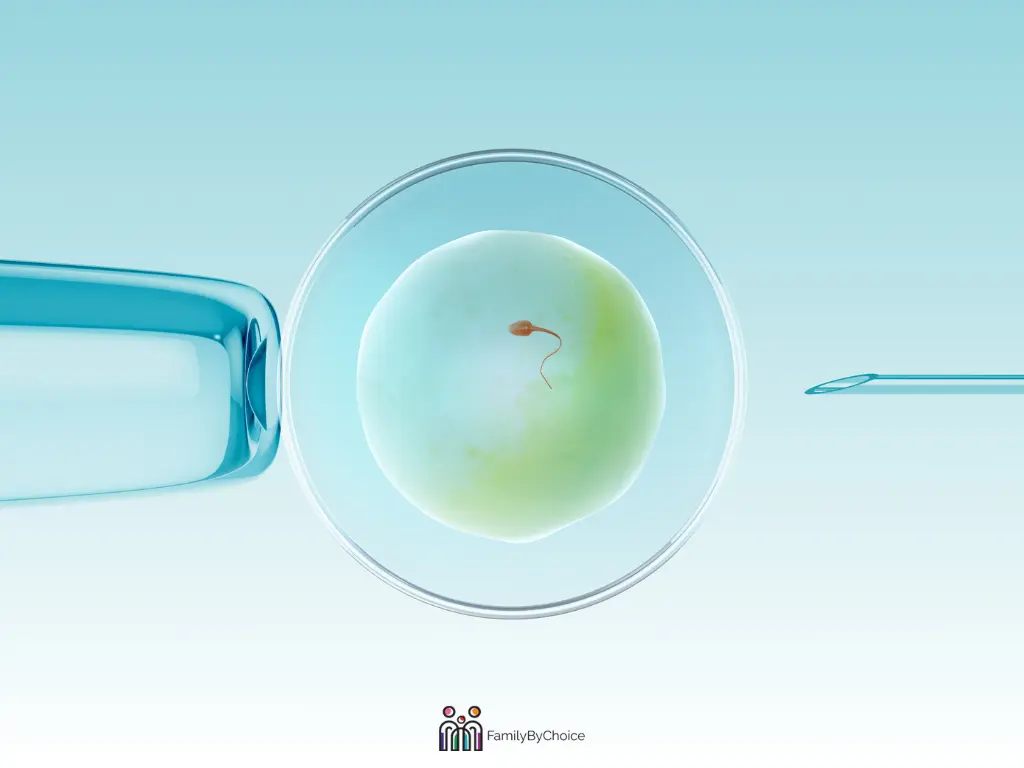
How IVF with Donor Eggs Works, Step by Step
At its core, IVF with donor eggs is exactly what the name suggests: eggs from a donor are fertilized with sperm in a laboratory, and the resulting embryo is transferred into the recipient’s uterus, where it can implant and develop into a pregnancy.
The process involves two people doing separate (but coordinated) things: the egg donor, whose ovaries are stimulated to produce eggs, and the recipient (you), whose uterine lining is prepared to receive the embryo. When you use frozen donor eggs, which is increasingly common and equally effective, the donor has already completed her cycle before yours begins, which removes the need for any coordination.
Here is the complete journey.
Step 1: Initial consultation and medical screening (weeks 1–4)
Before anything else, you’ll meet with a reproductive endocrinologist (RE) a specialist in fertility medicine. This consultation is where your individual situation is fully assessed and a personalized treatment plan is created.
For the recipient, initial testing typically includes:
- Hormone tests: Estradiol and progesterone to understand your baseline and rule out conditions that could affect the uterine environment
- Uterine evaluation: A transvaginal ultrasound to assess the shape, size, and lining of the uterus. In some cases, a saline infusion sonogram (SIS) or hysteroscopy is performed to look for polyps, fibroids, or other conditions inside the uterine cavity that could affect implantation
- Infectious disease screening: HIV, Hepatitis B and C, syphilis, rubella immunity, CMV status, and others, depending on your country
- Thyroid and autoimmune screening: Conditions like hypothyroidism or certain autoimmune disorders can interfere with implantation and are treatable
For a male partner:
- Semen analysis: Evaluating sperm count, motility, and morphology to determine whether standard fertilization (IVF) or intracytoplasmic sperm injection (ICSI) is needed
Psychological counseling is required before starting donor egg IVF at most reputable clinics worldwide. This isn’t a formality. It’s a meaningful conversation with a counselor who specializes in reproductive medicine, covering the emotional and relational implications of using donor genetic material, how you might talk to a future child about their origins, and how you’re both coping so far. Many people find it genuinely helpful.
Some clinics also offer a mock transfer cycle, a practice run in which your uterine lining is prepared with hormones and measured without an actual embryo transfer. This confirms your body responds as expected and allows the team to refine your medication protocol before the real cycle begins.
Step 2: Choosing your egg donor
Egg donor selection is, for many people, one of the most emotionally charged parts of the entire process. We’ve dedicated a full section to it below, but here’s a summary of what happens at this stage:
You will work with your clinic, egg bank, or donor agency to identify a donor who meets your preferences and medical criteria. Depending on the type of donor program and country, this may involve browsing a database of detailed profiles, or working with a coordinator who helps match you based on your characteristics and preferences.
When frozen eggs are used, selection can sometimes happen within days to weeks. When fresh donor eggs are used, matching and scheduling typically takes several months.
Step 3: The donor’s cycle: stimulation and egg retrieval (10–14 days)
While you are preparing your uterine lining (see Step 4), the egg donor goes through the active, medical part of the process.
Ovarian stimulation (10–12 days):
The donor self-administers daily injectable hormone medications, typically a combination of FSH (follicle-stimulating hormone) and LH (luteinizing hormone), to stimulate her ovaries to develop multiple follicles simultaneously. Normally, the body matures one egg per cycle; stimulation produces many more.
Every 2–3 days during stimulation, the donor comes in for monitoring appointments: transvaginal ultrasound to measure follicle growth, and blood tests to check estradiol levels. When the follicles reach approximately 16–18mm in diameter, a “trigger shot” is given – an injection of hCG (human chorionic gonadotropin) or a GnRH agonist, which initiates the final maturation of the eggs. Egg retrieval is scheduled precisely 36 hours later.
Egg retrieval (~20–30 minutes):
The egg retrieval procedure is performed under intravenous sedation. The donor is comfortable and unaware of the procedure. Using a transvaginal ultrasound probe, the doctor guides a fine needle through the vaginal wall into each ovarian follicle and gently aspirates the fluid, which contains the eggs. There are no incisions.
The embryologist in the adjacent laboratory immediately examines the fluid to identify and isolate the mature eggs. A typical fresh donor cycle yields 10–20 mature eggs.
The donor recovers in a rest area for a few hours, then goes home. Temporary bloating, cramping, and fatigue are normal for a few days.
When you use frozen donor eggs, this step has already happened. The eggs were retrieved from the donor in a previous cycle, vitrified (flash-frozen), and are now stored at the egg bank, waiting to be shipped to your clinic and thawed when your uterus is ready.

Step 4: Preparing your body (endometrial preparation)
This is your active medical phase. While the donor’s eggs are being retrieved (or while frozen eggs are being thawed and fertilized), your job is to prepare your uterus to receive an embryo. This is called endometrial preparation or endometrial priming.
The endometrium is the tissue that lines the inside of the uterus. Every month, it thickens in response to hormones and then sheds (the menstrual period) if no embryo implants. In a donor egg cycle, you use hormone medications to recreate this process under controlled conditions without needing to ovulate yourself.
Phase 1: Estrogen (2–3 weeks):
You begin taking estrogen, usually as oral tablets, skin patches, or vaginal tablets. Estrogen causes the endometrial lining to thicken. Your clinic will monitor your progress with transvaginal ultrasound appointments every few days.
The goal is to achieve a lining of at least 7–8mm (the optimal range is 9–14mm) with a specific appearance on ultrasound called the “trilaminar” or “triple-line” pattern. This pattern indicates the lining is ready to receive an embryo.
Phase 2: Progesterone:
Once your lining reaches the right thickness and pattern, you begin progesterone. Progesterone transforms the lining into its “receptive” phase, the window during which an embryo can implant. It is typically given vaginally (pessaries or gel) or, in some protocols, as intramuscular injections.
The timing here is critical. For a blastocyst (day-5 embryo) transfer, the embryo is transferred exactly 5 days after progesterone starts. This mimics the precise window of natural implantation.
Both estrogen and progesterone continue through the first trimester (approximately 10–12 weeks of pregnancy), after which the placenta takes over hormone production.
For women who have already gone through menopause or have no ovarian function: the protocol is usually simpler and more straightforward, since there’s no natural cycle to suppress first.
For women who still have ovarian function: the clinic may prescribe a brief course of birth control pills or a GnRH agonist (like Lupron) first, to prevent spontaneous ovulation from disrupting the timing.
Step 5: Fertilization and embryo culture in the lab (days 1–6 after retrieval)
On the day of retrieval, or on the day frozen eggs are thawed, the eggs are fertilized with sperm from your partner (or a sperm donor, if needed).
Two fertilization methods exist:
Standard IVF insemination: Sperm and eggs are placed together in a dish and sperm fertilize the eggs naturally. Used when sperm parameters are normal and fresh donor eggs are being used.
ICSI (intracytoplasmic sperm injection): A single sperm is injected directly into each egg using a microscopic needle. ICSI is always required when frozen donor eggs are used, because the freezing process slightly hardens the outer shell of the egg (zona pellucida), making natural penetration by sperm more difficult. ICSI is also used whenever there are any concerns about sperm parameters.
Fertilization is assessed 16–18 hours later. About 70–85% of mature eggs fertilize successfully.
Embryo development over 5–6 days:
The embryologist monitors the embryos daily in a specialized incubator. The stages are:
- Day 1: Fertilization confirmed (the egg now has two pronuclei: one from the egg, one from the sperm)
- Day 2–3: Cleavage stage: cells divide to 4, then 8 cells
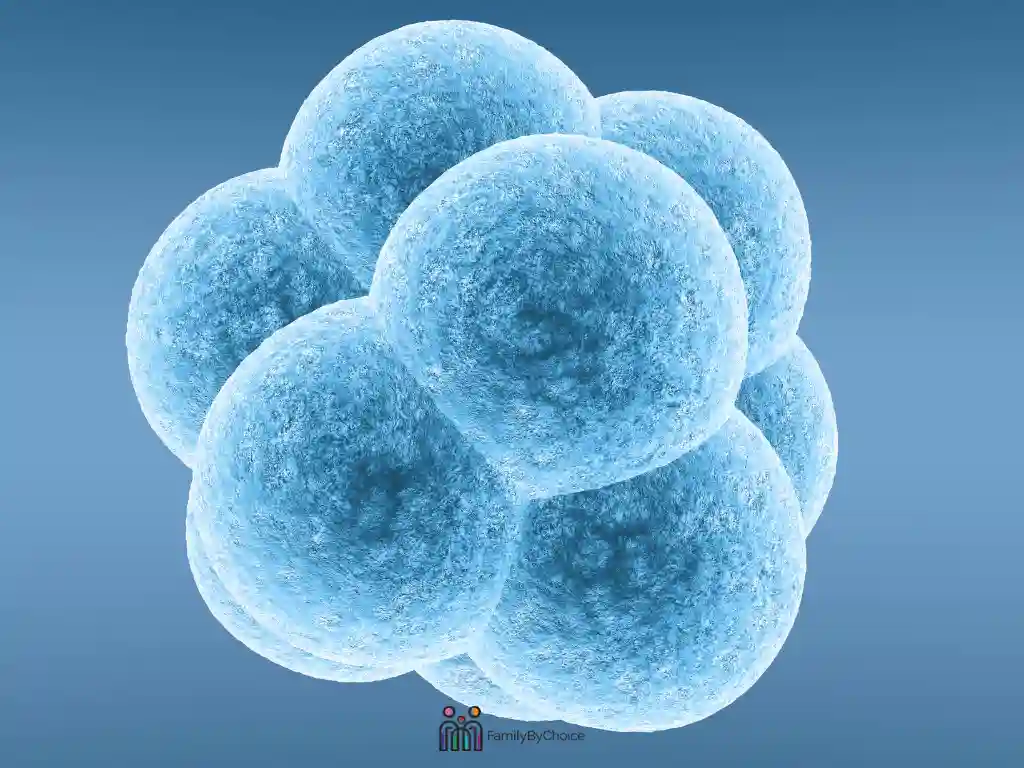
- Day 5–6: Blastocyst stage: a fluid-filled cavity forms and the embryo now has 100+ cells organized into distinct inner and outer layers
Blastocyst-stage transfer is now standard because embryos that reach blastocyst have already demonstrated strong development, and the transfer timing better matches the natural window of uterine receptivity. Approximately 50–60% of fertilized eggs reach the blastocyst stage.
Optional: Preimplantation Genetic Testing (PGT-A)
PGT-A involves biopsying a few cells from each blastocyst and testing them for chromosomal abnormalities (aneuploidy). The goal is to transfer only chromosomally normal embryos, reducing the risk of miscarriage and failed implantation.
For donor egg embryos, PGT-A is somewhat more nuanced than in own-egg IVF. Because the donor is typically young and healthy, the baseline aneuploidy rate is already lower than it would be with an older egg; approximately 20–25% of embryos from donors aged 20–30 may have chromosomal errors. Whether PGT-A is worth the additional cost ($3,000–$6,000 per batch) depends on factors like how many embryos you have, your history of miscarriage, and your doctor’s recommendation. It is not universally recommended for donor-egg cycles, but it can offer important peace of mind for some families.
Step 6: Embryo transfer day
Embryo transfer is a simple, brief procedure. Most people describe it as similar to a cervical smear or Pap test.
You will lie on an examination table. Your doctor uses a thin, flexible catheter to gently guide the embryo through your cervix and deposit it into the optimal position within the uterine cavity. The whole procedure takes about 5–10 minutes and requires no anesthesia.
The embryo is loaded into the catheter in the laboratory moments before the transfer, and an ultrasound probe on your abdomen confirms the placement.
You will see the embryo on a screen before transfer – a tiny glowing dot. Many people describe this moment as unexpectedly emotional.
How many embryos should be transferred?
In most countries and most clinics, single embryo transfer (SET) is now the strong recommendation from both ASRM and ESHRE, especially with donor egg embryos that have demonstrated good development. Transferring two embryos dramatically increases the risk of twins, which carries a 2.5x higher risk of pre-eclampsia, significant risk of preterm birth, and other serious complications. With good-quality donor egg embryos, success rates with SET are excellent, there is usually little benefit to transferring two, and meaningful risk.
If you have additional embryos of good quality, they can be vitrified (frozen) for use in future cycles.
After the transfer, you rest briefly (usually 15–30 minutes) and then go home. Normal light activity is fine; there is no evidence that bed rest improves outcomes.
Step 7: The two-week wait and pregnancy confirmation
The 9–14 days between embryo transfer and the first pregnancy blood test are, for most people, the hardest part of the entire process. You are waiting, and there is nothing medical you can do to influence the outcome. This period has been given its own name in the fertility community – the “two-week wait” or 2WW, and it deserves acknowledgment.
You will likely experience physical symptoms during this time: bloating, cramping, breast tenderness, fatigue, spotting. The difficult truth is that all of these can be caused either by the progesterone medication (which mimics pregnancy symptoms) or by early pregnancy itself. It’s genuinely impossible to tell the difference from symptoms alone. Home pregnancy tests during this window are unreliable and can be misleading.
The definitive test is a blood beta-hCG test, usually 9–14 days after transfer. A positive result, with a specific minimum level and then a doubling of that level 48 hours later, confirms early pregnancy. The first ultrasound to confirm a heartbeat typically takes place around 6–7 weeks of pregnancy.
If the result is negative, your clinic will schedule a consultation to review what happened and discuss next steps. A failed cycle is not the end of the story, and we address this fully later in this guide.
Fresh vs. Frozen Donor Eggs: How to Decide
You’ll encounter two options when exploring donor eggs: fresh (retrieved from a donor whose cycle runs in parallel with yours) and frozen (already retrieved, vitrified, and stored at an egg bank, ready when you are).
Both are excellent! The right choice depends on your timeline, budget, and priorities. The game-changer was vitrification, an ultra-rapid freezing technique developed in the mid-2000s that flash-freezes eggs so quickly that damaging ice crystals never form, achieving a ~95% post-thaw survival rate.
ASRM declared the technology no longer experimental in 2013, and frozen cycles now outnumber fresh ones in the US. In practical terms: fresh cycles typically yield more eggs (15–25+), more potential embryos, and suit those wanting maximum future options or using a known donor, but take 3–6 months to coordinate and cost significantly more.
Frozen cycles offer faster starts (days to weeks), lower cost, and scheduling flexibility, particularly useful if you’re travelling abroad for treatment, though you’ll work with a smaller initial batch (typically 6–8 eggs per lot). On outcomes, the ASRM’s 2021 guideline is clear: “There are no significant differences in per-transfer pregnancy rates with cryopreserved versus fresh donor oocytes.” Don’t let anyone tell you frozen is second best.
Donor Selection: What Intended Parents Should Know
Choosing a donor is one of the most deeply personal decisions in this entire process. There’s no objectively right or wrong choice – what matters is finding someone you feel comfortable with, within the options your clinic or egg bank offers.
Here’s what you need to understand.
Types of donors
Anonymous donors: The donor’s identity is never disclosed to the recipient or to any child born. This is legally mandated in many European countries including Spain, the Czech Republic, North Cyprus, and Bulgaria. In these countries, you will receive detailed medical and physical information about the donor, but no identifying information and no photos.
Open-ID (identity-release) donors: The donor agrees, at the time of donation, that when any child born from her eggs turns 18, that child may request identifying information. This is now legally required in the UK (since 2005), Sweden (since 1984), Australia, New Zealand, Portugal, Austria, Finland, and several other countries. In the United States, open-ID donation is available but not legally mandated in most states.
Known donors: A friend, sibling, or other person known to you personally volunteers to donate eggs. The same medical screening applies, and strong legal contracts are essential to clarify parental rights and expectations for all parties. Known donation involves unique emotional dynamics that benefit from careful psychological support for everyone involved.
Egg donor agencies vs. egg banks vs. clinic programs
Egg donor agencies (most common in the US): Independent companies that recruit, screen, and manage egg donors. They maintain large online databases of donor profiles, including detailed personal statements, photos, and medical histories. Intended parents browse these and select who they’d like to work with. The agency coordinates the fresh cycle. Agency fees typically range from $5,000–$10,000 on top of all other costs. Timeline: approximately 3–6 months from initial inquiry to retrieval.
Egg banks: Organizations that recruit and screen donors, perform egg retrievals, freeze the eggs using vitrification, and sell them in lots (typically 6–8 eggs per lot) to clinics worldwide. The eggs are ready immediately. Egg banks typically ship eggs to your chosen clinic. There are no agency fees; the cost is built into the lot price.
Clinic in-house programs: Some fertility clinics run their own donor recruitment programs, with no separate agency involved. This can reduce cost and streamline coordination. The donor pool is smaller, but the entire process stays within one team.
What’s in a donor profile
The information included in a donor profile varies by country and program, but typically includes:
- Physical characteristics: height, weight, hair color, eye color, skin tone, ethnicity
- Blood type
- Education and professional background
- Hobbies and personal interests
- A personal statement written by the donor
- 3-generation family medical history
- Results of genetic carrier screening
- Psychological evaluation summary
- Reproductive history (prior donation cycles and outcomes, if any)
- Childhood and/or adult photos (in countries where this is permitted)
In countries where anonymity is legally required (Spain, Czech Republic, etc.), you will typically receive extensive physical, educational, and medical information but no photos and no identifying details. This is different from the US and UK models, but the genetic screening standards are equally thorough.
What screening donors go through
Egg donors at reputable programs undergo one of the most thorough medical evaluations in reproductive medicine:
- Medical history review: Complete personal and family medical history, reviewed by a genetic counselor
- Genetic carrier screening: Typically tests for 200–300+ genetic conditions, including cystic fibrosis, spinal muscular atrophy, fragile X syndrome, sickle cell disease, and others. This is done to ensure the donor doesn’t carry two copies of a recessive gene, and to allow you to check whether you carry the same genes (if so, your embryos could be at risk)
- Karyotype: A chromosomal analysis confirming no significant chromosomal abnormalities
- Infectious disease testing: Mandatory testing for HIV, Hepatitis B and C, CMV, syphilis, chlamydia, gonorrhea, and others
- Ovarian reserve testing: AMH, antral follicle count, and baseline FSH to confirm the donor is likely to respond well to stimulation
- Psychological evaluation: Conducted by a licensed psychologist or counselor. This explores the donor’s motivations, emotional readiness, understanding of the implications, and psychological stability. Research suggests 2–27% of applicants are excluded for psychological reasons.
- Drug and substance screening
The ASRM recommends that donors be between 21 and 34 years of age, in excellent general health, and limited to a maximum of 6 donation cycles in their lifetime. Only approximately 10% of donor applicants pass all screening criteria at selective programs.
How long donor matching takes
- Frozen egg bank: You can select a donor, have eggs shipped, and begin your endometrial preparation within days to a few weeks
- Fresh agency cycle: Typically 3–6 months from selecting a donor to egg retrieval, once matching, medical screening of the donor, and cycle scheduling are complete
- Clinic in-house program: Varies; waiting lists can apply, particularly if your donor pool is small or specific characteristics are requested

Success Rates: What the Data Says
Donor egg IVF has some of the highest success rates of any fertility treatment available, and the key reason is straightforward: it’s the donor’s age, not yours, that determines egg quality. Because donors are typically aged 21–34, the age-related decline in egg quality that drives down own-egg IVF success simply doesn’t apply.
The CDC states this explicitly in its annual ART report: “An intended parent’s age does not substantially affect success when using donor eggs.” What does change with recipient age is obstetric risk during pregnancy, not the chance of the embryo implanting.
Always look for live birth rate per embryo transfer when evaluating clinic statistics, not pregnancy rates, not cycle start rates. Live birth is the only number that tells you the chance of taking a baby home.
SART and CDC 2022 national data show donor egg live birth rates of 45–55% per transfer for recipients under 43, dropping modestly to 30–40% for those over 43, compared to just 3–5% with own eggs at the same age. The HFEA’s donation report puts this in stark relief: birth rates with own eggs for patients aged 43–50 sit at around 5%, while donor eggs keep birth rates above 30% across all age groups – roughly a sixfold improvement.
A single transfer gives you a 40–55% chance. Additional transfers using frozen embryos from the same cycle compound that probability significantly: cumulative success after 3–4 transfers typically reaches 75–95%.
Miscarriage rates also improve: because donor eggs come from younger donors, chromosomal abnormalities are far less common, bringing miscarriage rates down to approximately 10–16% for donor egg recipients over 40, compared to 30–50% with their own eggs at the same age.
Risks and Side Effects
IVF with donor eggs is well-established and generally safe, but going in fully informed makes the process easier to navigate.
For the egg donor, the primary risk is ovarian hyperstimulation syndrome (OHSS), where the ovaries over-respond to stimulation medication. Mild OHSS (bloating, discomfort) is common and self-resolving.
According to ASRM’s 2023 guideline, moderate-to-severe OHSS occurs in approximately 1–5% of stimulation cycles, with severe cases requiring hospitalization in under 1–2%, a rate that has fallen significantly with modern GnRH agonist trigger protocols.
The egg retrieval itself carries a small risk of bleeding or infection (serious complications occur in under 1% of retrievals). On long-term health: no established evidence links egg donation to early menopause, reduced fertility, or cancer risk, and the ASRM limits donors to a maximum of 6 lifetime donation cycles as a precautionary measure.
For the recipient, hormone medications commonly cause temporary side effects: headaches, nausea, breast tenderness, bloating, and fatigue, that resolve after the cycle. The most important risk to understand is pre-eclampsia. A meta-analysis published in the American Journal of Obstetrics & Gynecology (Masoudian et al.) found pre-eclampsia rates of approximately 10.7% in donor egg singleton pregnancies, compared to 2–4% in own-egg IVF, likely because the embryo shares none of the birth mother’s DNA, which may affect immune tolerance. A separate meta-analysis (Blázquez et al., PMC) found a relative risk of 2.62 versus own-egg IVF.
The practical implication: donor egg pregnancies should be managed as higher-risk from the outset, with obstetric-led care, regular blood pressure and urinalysis monitoring, and a conversation with your doctor about low-dose aspirin in the first trimester. Pre-eclampsia caught early can be managed safely. The key is knowing to look for it.

The Emotional Side: What No Clinic Brochure Tells You
Medical steps and statistics are important, but they’re only part of what you’re navigating. The emotional experience of donor egg IVF is profound, complex, and deeply individual. This section is for the parts that aren’t in the protocol.
Epigenetics: your body shapes your baby
One of the most powerful and scientifically substantiated things we can tell you is this: carrying a pregnancy with donor eggs makes you far more than a vessel for someone else’s genetics.
Epigenetics is the study of how environmental factors influence which genes are expressed, and essentially, how genes are turned on or off without changing the DNA sequence itself. Research in this field has revealed something extraordinary about donor-egg pregnancy.
A study published in the journal Development (Vilella et al., 2015) found that the endometrium, your uterine lining, releases small vesicles called exosomes that are absorbed by the pre-implantation embryo. These exosomes contain maternal microRNAs that enter the embryo and can modify which genes are expressed in early development. In other words, your body is communicating with the embryo from the very beginning of its existence, before implantation even occurs.
Beyond this, throughout the nine months of pregnancy, your nutritional state, hormonal environment, stress responses, and physical health all influence the epigenetic patterning of your developing baby – affecting metabolism, brain development, immune function, and more. Research has shown that DNA methylation patterns differ between donor-egg and own-egg embryos in ways that reflect the birth mother’s influence.
We want to be careful to represent this science accurately: epigenetics cannot alter the DNA sequence itself. Your child will still carry the egg donor’s genetic code and the sperm provider’s genetic code. What changes is how those genes are expressed and your body is one of the most powerful forces shaping that expression.
Many parents find this deeply meaningful. You are not a passive participant. Your body is doing something extraordinary for your child from the very first moment.
Bonding fears and what the research shows
“Will I bond with this baby?” is perhaps the most common fear expressed by people considering donor egg IVF. It is also, according to decades of family research, overwhelmingly unfounded. Not because the fear is irrational, but because the reality almost universally turns out to be nothing like the fear.
The Cambridge Longitudinal Study, led by Professor Susan Golombok of the University of Cambridge, is the most comprehensive long-term study of families created through assisted reproduction. Published in Developmental Psychology in 2023, following children conceived via donor eggs, donor sperm, and surrogacy from infancy through age 20, the study consistently found:
- No meaningful difference in psychological well-being between donor-conceived and naturally-conceived children at any age
- Egg-donation mothers showed more positive parent-child relationships in warmth and enjoyment than mothers of children conceived naturally, at ages 1, 2, and 3
- Children in egg-donation families rated their relationships with parents as significantly higher in warmth than children in standard IVF families
Professor Golombok summarized the findings this way: the strong desire to have a child, and the active effort parents make to meet that desire, seems to be more important to family functioning than the genetic connection itself.
Bonding is built not in the moment of genetic conception, but in the ten months of pregnancy, the skin-to-skin hours after birth, the midnight feeds, the years of play and presence and love. Genetics influences certain traits. Parenting builds a person.
Telling your child and the people around you
The question of disclosure – whether and how to tell your child about their donor conception, is one of the most significant decisions you’ll face. Here’s where the research and professional organizations stand:
Professional consensus: Both ASRM and ESHRE strongly recommend telling children about their donor conception. The evidence supporting early disclosure is robust.
Timing matters: Children told about their origins before the age of 7 show more positive family relationships and higher well-being than those told later. Late disclosure, particularly in adolescence or adulthood, is associated with significant distress, feelings of betrayal, and disrupted family trust.
Secrecy is increasingly fragile: Consumer DNA testing services are accessible, inexpensive, and widely used. Children who are not told about donor conception increasingly find out anyway: through DNA matches with half-siblings or donor relatives. Discovering this information unexpectedly, rather than from a loving parent, can be deeply damaging. According to data from the Cambridge Longitudinal Study, 88% of egg-donation parents had disclosed to their children by the time the children were 20 years old.
What to say: There are excellent books written specifically for young children about donor conception – clear, loving, and age-appropriate. Organizations like the Donor Conception Network (UK) offer templates, workshops, and community support for navigating disclosure at every age.
Telling others: Who else you tell, extended family, friends, colleagues, is entirely your decision. Some families are open; others are private. Both approaches work. The important thing is that your child hears their story from you first, in a loving context, before they might hear it from elsewhere.
When a cycle fails: coping and next steps
Here is something we want to say clearly, because most guides don’t: the first transfer does not always work.
With donor eggs, live birth rates per transfer are roughly 40–55%. That means 45–60% of first transfers do not result in a pregnancy. This is not failure. This is the reality of a highly effective but not perfect medical process, and it happens to many people who eventually go on to have healthy children.
If your transfer results in a negative test:
Give yourself time to grieve. A failed cycle is a genuine loss – the loss of a specific embryo, the loss of hope that was building, the loss of the timeline you’d imagined. You don’t need to rush to “be okay.”
Ask for a review consultation. Your doctor will analyze what happened: Was the lining adequate? Were the medication levels appropriate? Were there any signals of a possible immune or anatomical issue? Sometimes adjustments to the protocol make a significant difference in subsequent cycles.
Consider your remaining options. If you have frozen embryos from the same cycle, a frozen embryo transfer (FET) can typically be done in the next or second cycle, usually at lower cost and with a shorter preparation period than a fresh cycle.
Know that cumulative odds are much better. Over 3–4 transfers, cumulative success rates with donor eggs typically reach 75–95%. The first negative test does not tell you the full story of your journey.
Seek support. Failed cycles are genuinely hard, and isolating yourself in that difficulty is common but not necessary. Fertility counselors, support groups (both in-person and online), and communities of people who’ve been through this can provide something medicine cannot: the knowledge that you are not alone.
A note for partners
If you are the partner of the person carrying the pregnancy, your experience in this journey is real and valid too, and often overlooked. You may be at a different stage of acceptance around donor eggs. You may feel helpless during the medical parts of the process. If one partner has a genetic connection to the child (through sperm) and the other doesn’t, this asymmetry can create unspoken tension.
Open communication, ideally supported by a counselor who specializes in fertility, strengthens relationships through this process. The goal is to arrive at parenthood as a team.
Pathways for Every Family
Donor egg IVF is not only for heterosexual couples. Every family configuration below has used this path to parenthood.
Heterosexual couples: The “standard” pathway described throughout this guide – recipient partner undergoes endometrial preparation; partner provides sperm.
Lesbian couples & reciprocal IVF: One partner provides eggs (or donor eggs are used if neither can), which are fertilized with donor sperm. The embryo is then transferred into the other partner’s uterus, the one who will carry the pregnancy. This is sometimes called ROPA (Reception of Oocytes from Partner) or co-IVF. It allows both partners to have a biological role. It is available in the UK, Spain, many US states, and a growing number of other countries.
Gay male couples: Donor eggs are fertilized with sperm from one (or both, in separate batches) partners, and the resulting embryo(s) are transferred to a gestational surrogate, who carries the pregnancy. This path requires both egg donation and surrogacy arrangements, both legal agreements, both requiring careful coordination. Several countries that permit egg donation restrict surrogacy, so legal guidance specific to your country is essential.
Single parents by choice: Single women may use donor eggs combined with donor sperm (sometimes called “double donation”). Single men follow the same path as gay male couples – donor eggs plus surrogacy. Single parenthood by choice is a growing and increasingly well-supported family structure, with specific community organization and globall groups.
Transgender and non-binary individuals: Fertility preservation options and treatment pathways depend heavily on individual medical history and transition status. Leading fertility centers explicitly welcome transgender and non-binary patients. Trans women who have not preserved their own sperm can use donor sperm; trans men who have transitioned but preserved eggs may not need donor eggs at all. Many combinations are possible. Look for a fertility clinic that has experience and affirming practice with gender-diverse patients.
Your Next Step
If you’ve read this far, you now know more about IVF with donor eggs than the vast majority of people who begin this process. That knowledge matters. It helps you ask better questions, make more informed decisions, and navigate the journey with greater confidence.
Here’s what we’d suggest as practical next steps:
1. Find a fertility specialist with experience in donor egg IVF. Not all fertility clinics offer donor egg programs, and the level of expertise and support varies significantly. Ask about their specific donor egg live birth rates, how they support recipients emotionally through the process, and what their cancellation rate is for fresh donor cycles.
2. Have an honest consultation about your uterine health. Even before selecting a donor, understanding whether your uterus is ready to receive an embryo is foundational. A baseline scan and hormone panel will give you clarity.
3. Start the emotional work early, not as an afterthought. Consider connecting with a counselor who specializes in fertility before you begin treatment. Not because there is something wrong, but because this is a significant journey and going into it with support is a gift to yourself.
4. If treatment abroad is something you’re considering, research the legal implications in your home country before committing. A reproductive lawyer consultation is a worthwhile investment.
5. Connect with the community. Hear from people who have been exactly where you are. Their experiences, honesty, and hope are invaluable. If you’d like to go deeper on the medical and emotional side of this journey, our IVF and fertility courses are designed specifically for intended parents – covering everything from understanding your test results to preparing emotionally for each stage of treatment.
You are not starting from zero. You are starting from a place of deep desire to build a family, and that is where the best journeys begin.
This article is educational in nature and is not a substitute for personalized medical advice. Success rates, costs, and legal regulations vary by country, clinic, and individual circumstances and may change over time. Always consult a qualified reproductive endocrinologist and, where relevant, a reproductive lawyer, before making decisions about your fertility treatment.
Family by Choice is an educational platform for intended parents. We do not endorse any specific clinic, agency, or egg bank.

