Traditional IVF fertility treatments in Europe also have clear limitations: IVF success rates typically range from 30–50% per embryo transfer, and the average cost of a single IVF cycle is generally €3,000–€7,000, depending on the country and clinic.
Patients often endure repeated injections, procedures, and long waits with no guarantee of success.
Now, thanks to modern data and computing power, artificial intelligence (AI) is poised to change this. AI – essentially machine learning algorithms trained on huge fertility datasets, can spot hidden patterns in genetic, hormonal, and imaging data. This means smarter use of the rich information generated during IVF, from sperm and egg quality to embryo growth, so that treatments are more precise and personalized than ever.
AI’s basic strength is in analyzing very large amounts of data and finding complex patterns that humans might miss. In fertility clinics today, we have time-lapse video of embryos, genetic screening results, hormone levels, and more – a treasure trove for AI.
By “learning” from thousands of cases, machine learning models can predict outcomes (for example, pregnancy success) and suggest the best treatment protocols. In practice, this can mean using patient-specific factors (age, hormone profile, genetics) to tailor IVF drug doses or cycle timing.
Experts note that now is an ideal time to integrate AI: computing is fast and affordable, and clinics are beginning to digitize their records and lab imaging, giving AI systems the fuel they need to learn. As one review puts it, AI in reproductive care “leverages large datasets to improve efficacy and reduce subjectivity,” touching every step from diagnostics to counseling.
In short, areas like embryo selection, sperm and egg analysis, genetic screening, and treatment planning stand to benefit the most from AI-driven advances.
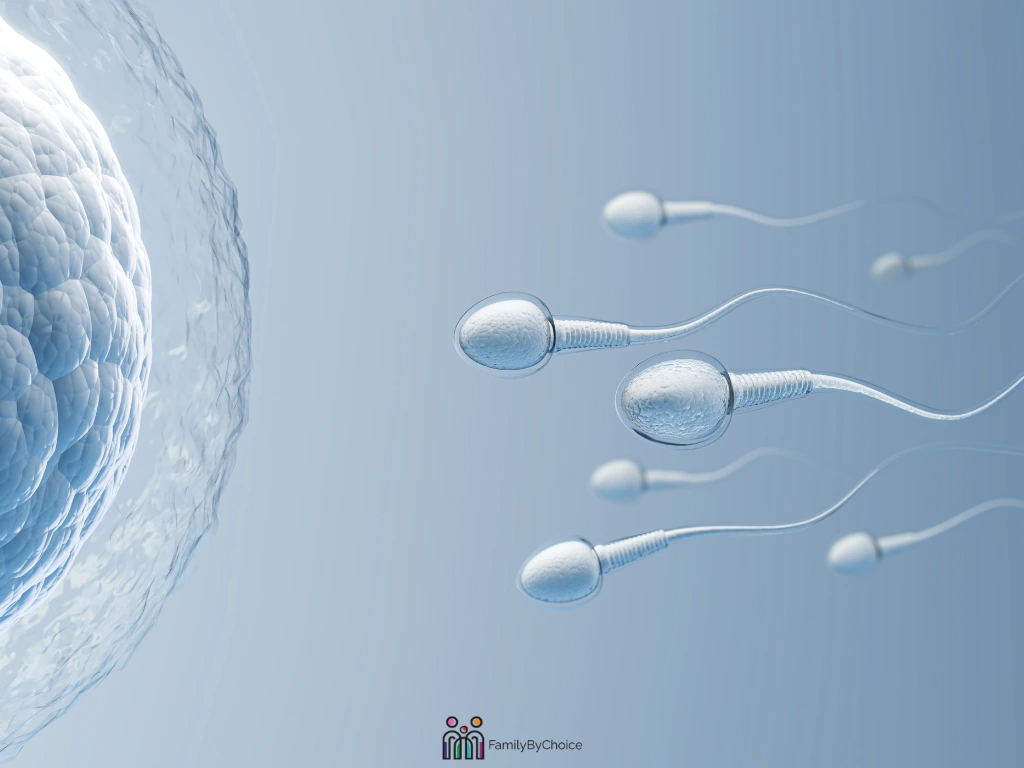
IVF and Embryo Selection – The Power of Prediction
Selecting which embryo to transfer is one of the hardest decisions in IVF. Traditionally, embryologists grade embryos by eye under a microscope, looking at shape and cell development.
This is partly art and partly science, and it can be subjective.
AI changes the game by quantifying that visual information. Machine learning models analyze thousands of embryo images and videos (often time-lapse data) along with known outcomes. The algorithms learn subtle features: growth patterns, cell divisions, even light intensity that correlate with viability.
For example, studies of AI tools like icONE and iDAScore show that they can predict implantation and pregnancy success with high accuracy. One multi-center study found an AI tool reached a 77.3% clinical pregnancy rate versus 50% using conventional selection.
Another tool, iDAScore, uses time-lapse footage to grade embryos automatically, matching embryologists’ rankings while saving 30% of lab evaluation time.
These AI systems do not “look” the same way people do; they can spot patterns imperceptible to the human eye. For example, one AI model picks up on internal cellular movements over hours of development, something a quick human glance could never catch. The result is more objective, data-driven embryo rankings.
In practice, this has translated to improved IVF outcomes in some clinics: patients may need fewer transfer attempts, and more transfers end in pregnancy when AI guidance is used.
Tools like iDAScore or Life Whisperer illustrate this difference from traditional grading. Instead of a doctor assigning a visual grade, AI processes images through neural networks.
iDAScore, for example, uses a time-lapse incubator video and gives each embryo a numerical score. Life Whisperer (an AI system by an Australian company) can take a single standard microscope photo of a day-5 blastocyst and estimate its viability.
These systems incorporate data from many sources: image features, patient factors or even genetic test results to make a prediction. In contrast, traditional grading relies on fixed criteria (number of cells, symmetry, fragmentation) and intuition.
By standardizing analysis and quantifying risk, AI tools reduce the subjectivity and variability between clinics and technicians. In sum, machine learning–based embryo selection represents a significant leap: it transforms embryo quality assessment into a predictive science, often improving success rates of IVF cycles.
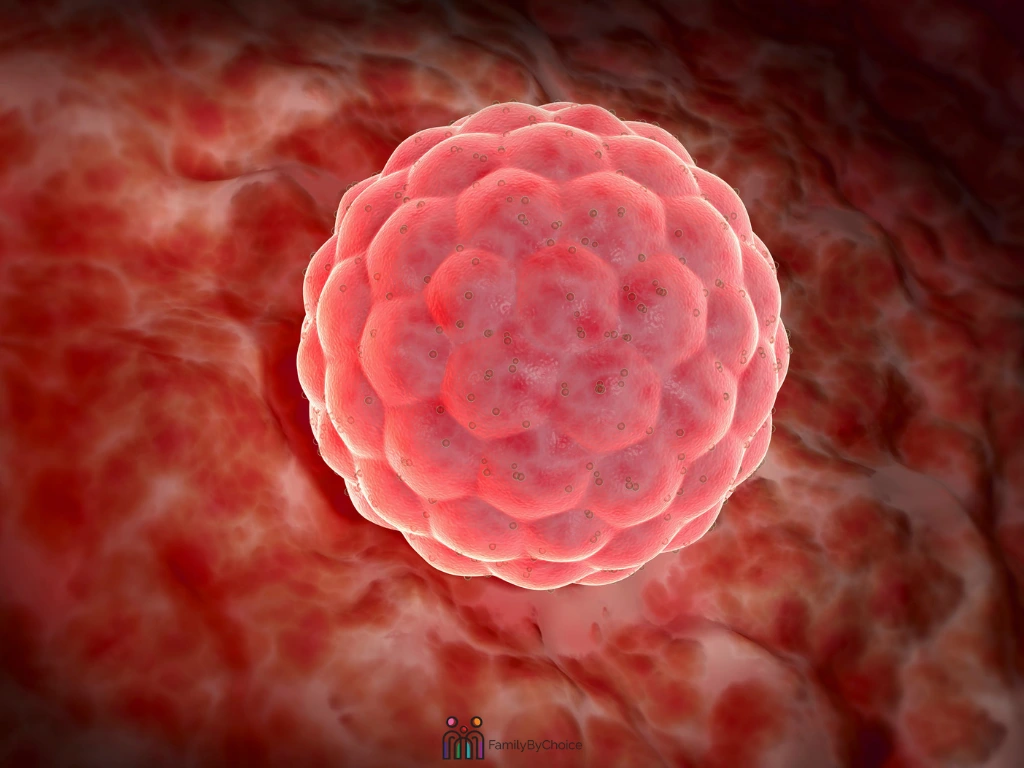
AI in Sperm and Egg Analysis
AI is also lending a hand at the very start of the IVF process, by helping embryologists evaluate sperm and eggs. For sperm analysis, computers have long been used to track motility, but AI takes it further.
Advanced image analysis algorithms can examine video of sperm under the microscope and more precisely measure how each one moves and what it looks like.
Studies find that AI assessment of sperm motility and shape can be about 15% more accurate than human evaluation. This means AI can flag subtle motion abnormalities or morphological defects that a lab technician might miss on a quick look. Some systems even automatically sort or recommend the healthiest-looking sperm for procedures like intracytoplasmic sperm injection (ICSI).
Similarly, AI is starting to be applied to eggs (oocytes). An embryologist’s judgment of egg quality (based on appearance of the cell and surrounding cells) can vary. AI models trained on large datasets of egg images and patient outcomes are being developed to predict which eggs are mature and likely to fertilize successfully.
In effect, AI algorithms can “learn” what a good egg looks like in ways beyond simple visual cues. More generally, AI integration spans many steps: it can classify sperm samples, assess oocyte quality, and even track lab workflows to reduce errors.
The common theme is that AI brings greater consistency and precision to tasks that traditionally relied on subjective human judgment. For example, one review notes that well-trained AI models help embryologists make faster, more objective selections of gametes and embryos.
In practice, this reduces inter-observer variability: instead of a score that depends on which lab tech is viewing the sample, AI gives a reproducible, data-driven assessment.
Overall, embryology labs report that AI tools make sperm and egg analysis more reliable. Clinics using AI have found that automated sperm sorting can yield higher fertilization rates. And while fully automated oocyte selection is still emerging, research suggests it’s only a matter of time before AI algorithms routinely advise on egg maturity. By taking the “guesswork” out of gamete evaluation, AI helps labs make each IVF attempt count more.
Personalization and Protocol Optimization
Perhaps the most exciting role for AI is making IVF treatments 100% personalized.
No two patients are alike, yet traditional IVF “recipes” use a one-size-fits-all approach. AI changes that by tailoring the protocol to individual needs.
Before an IVF cycle starts, machine learning systems can sift through a patient’s entire medical and reproductive history: age, AMH hormone levels, previous cycle responses, genetic markers, BMI, and more, to recommend the optimal stimulation plan.
For example, AI can suggest the exact starting dose of follicle-stimulating hormone (FSH) for ovarian stimulation that maximizes egg yield while minimizing risk of overstimulation.
This isn’t guesswork. One AI-driven study in a real-world clinic setting showed that doctors using an AI tool were able to significantly lower both the starting and total FSH doses for patients without reducing egg quality. In other words, the AI helped each patient get “just enough” medication, reducing costs and side effects. More broadly, AI-optimized protocols have already reduced FSH usage by up to 20% on average in some reports.
Behind the scenes, AI models also continuously adjust treatment during a cycle. Some decision-support systems predict the best day to trigger final egg maturation or suggest whether to extend or shorten stimulation.
In one research, an AI algorithm used data from over 19,000 patients to find the ideal follicle sizes for triggering IVF. By aiming for that optimal range, clinics improved the number of mature eggs retrieved and even saw higher live birth rates. This is powerful: instead of stopping stimulation on a fixed schedule, doctors now have data-driven insights on when each patient’s body is most ready.
All of this personalization addresses key infertility challenges. For example, patients who had “poor ovarian response” in the past may have a better chance with an AI-suggested protocol, and those at risk of ovarian hyperstimulation can avoid excessive medication.
Early evidence suggests that individualized IVF plans guided by AI can shorten time to pregnancy and reduce the number of required cycles.
AI brings a level of customization to fertility care that was previously only possible through trial and error. It “transforms an art into a science,” ensuring each couple or individual gets a protocol optimized for their unique situation.

Ethical and Clinical Integration Challenges
As with any new technology, introducing AI into fertility care raises important ethical and practical questions. Couples and clinicians alike may wonder: Who is responsible for AI-guided decisions? In practice, doctors retain ultimate clinical responsibility. AI should be viewed as an “assistant,” not an oracle. Experts emphasize that any AI recommendation must be transparent and interpretable. Patients should be fully informed when AI is part of their care, so they understand how and why decisions (like embryo ranking or dosage) are made.
Informed consent now includes explaining that “an algorithm” is helping guide the treatment and outlining its known benefits and limitations.
Bias and data privacy are other concerns.
AI models learn from existing data, so if that data has biases (for example, underrepresentation of certain ethnic groups or body types), the AI’s advice might unintentionally favor one group.
Strict regulatory frameworks and diverse datasets are needed to ensure fairness. For instance, laws like HIPAA govern patient data privacy in IVF clinics, and similar rules apply to genetic information. Reputable fertility centers will anonymize and secure any data used for AI training. Researchers also follow emerging guidelines (like the TRIPOD-AI framework) for transparent reporting of AI studies, to make sure tools are properly validated before clinical use.
Clinicians face their own integration challenges. Embryologists and doctors need training to use AI tools correctly and to interpret their output. There may be skepticism or fear of new tech. To address this, many clinics start with hybrid approaches: AI suggests a ranking, but an embryologist reviews it.
Over time, as confidence in the tool grows, clinics may rely on it more.
Importantly, AI is unlikely to replace human expertise. It augments it by handling routine analysis and flagging cases that need special attention, but it will never replace human expertise.
Equity and access are ethical considerations. Advanced AI systems may require expensive hardware or licensing, potentially limiting them to well-funded clinics. Industry and regulators must ensure that these innovations don’t widen the gap in fertility care.
For example, open-source AI tools and collaborative data-sharing could help smaller clinics benefit. In all cases, trust in AI depends on rigorous testing. As one expert notes, promising AI tools must undergo prospective clinical trials before we assume they improve outcomes. In practice, this means fertility centers integrate AI gradually, continually monitoring real-world success and being transparent with patients. When done thoughtfully, AI holds immense potential, but it must always be guided by human judgment, ethics, and care.
Where Is AI in Fertility Headed?
Looking ahead 5–10 years, the role of AI in reproductive medicine is likely to expand dramatically. We may see fertility clinics become partly virtual, with AI-powered apps guiding patients through each step of the journey.
Imagine a future where a woman uses a home monitoring device that tracks hormone levels or follicle growth, feeds that data to an AI cloud service, and receives real-time advice on medication timing, all from her living room.
Some fertility apps already use basic decision trees for timing, and AI could soon make them far more sophisticated. While “full-cycle virtual clinics” (from assessment to egg retrieval remotely) may still be years away, incremental steps are visible: telemedicine consultations supported by AI analytics, home urine hormone sensors, even remote embryo monitoring.
In the lab, advances continue.
We expect more automated IVF systems combining robotics, AI, and microfluidics. For example, time-lapse incubators with built-in AI will monitor embryos continuously and select the best ones without a human peeking under a microscope.
Electronic witnessing and tracking systems (already used to prevent sample mix-ups) will tie into AI databases, reducing human error further. The vision is an “intelligent incubator” that controls temperature, humidity, and even minor movements, all while analyzing embryos in real time.
By combining robotics (for handling tasks like precise injections) and AI (for decision support), the entire IVF process could become more standardized and efficient.
But, this does not replace human compassion. Doctors and nurses will still be needed to provide support, but it will relieve them of repetitive tasks and let them focus on patient care.
Could AI one day predict a woman’s reproductive lifespan or exact egg reserve? In theory, yes, by integrating longitudinal health data.
For example, algorithms might analyze patterns in hormone levels, genetic markers, and imaging to estimate how many viable eggs remain or when menopause will occur. Research in this area is emerging, but it’s important to be cautious: reproductive biology is complex, and such predictions would always come with uncertainty.
Still, if AI can learn from large studies of fertility over decades, it might one day give personalized timelines or flag early menopause risk, helping people make informed family-planning decisions earlier.Throughout all this, one thing will remain: the human core of fertility care. AI tools will become more powerful, but empathy and support will always be central to reproductive medicine. For hopeful parents, AI is simply another tool giving them clarity and confidence.
By predicting which embryos are healthiest, how to tune medications, or what outcomes to expect, AI can reduce anxiety and shorten the wait. Early evidence and expert consensus agree: when used responsibly, AI makes fertility care more accurate and personalized, helping many more individuals and couples realize their dream of parenthood.
As technology and regulation evolve together, the future of reproductive medicine looks to be a partnership, deeply human and deeply data-driven, guided by both empathy and innovation.
The Future of Fertility Is Smarter, More Personal – And Already Here
Artificial intelligence isn’t replacing reproductive medicine. It’s upgrading it. What once depended on intuition, limited data, and trial-and-error now has the support of powerful predictive tools that help patients get clearer answers, more tailored treatments, and, for many, a faster path to parenthood.
But understanding AI in fertility can feel overwhelming. The science moves quickly, clinics use different tools, and patients are often left trying to decode algorithms and acronyms while also navigating an emotionally demanding journey.
You shouldn’t have to figure this out on your own.
If you want to understand how AI is really being used in IVF labs, how clinics apply embryo-selection algorithms, what ethical safeguards exist, and what future breakthroughs could mean for your family-building plans, we created a fertility course Artificial Intelligence (AI) in Fertility: Transforming Reproductive Medicine.
The goal is simple: to help you make informed, confident decisions in a rapidly evolving field.
Join the Family By Choice membership to access the full course and get equipped with the knowledge you need to navigate AI-powered fertility care with clarity and confidence.
Related Articles:
Understand IVF success rates. Learn what live birth rates really mean, how clinics report results, why age, embryo quality, PGT-A, and transfer strategy matter, and how to read IVF statistics with confidence when planning your fertility journey.
Deciding between conventional IVF insemination and intracytoplasmic sperm injection (ICSI) can be overwhelming for future parents. In this article, we’ll explain what each method involves, their benefits and limits.
IVF Failed: What Are Your Real Next Options
IVF failed? Understand your real next options: from trying IVF again to donor eggs, surrogacy, or stepping back. A clear, compassionate guide helping intended parents make informed decisions after an unsuccessful cycle.
How to Start Surrogacy with Donor Eggs
Considering surrogacy with donor eggs? This comprehensive guide explains the medical process, who typically chooses this path, IVF steps, success rates, legal considerations, and costs.

