The Conversation Nobody Had With You, Until Now
When you were diagnosed, did anyone tell you that you could still be a dad?
If the answer is no, you’re not alone. And this article is the conversation you should have had.
For many HIV+ gay men, there’s a moment that happens quietly, without ceremony, somewhere in the fog of a diagnosis. Nobody announces it. Nobody writes it down. But something shifts, a door closes, and the idea of biological fatherhood just stops feeling like a possibility.
Not because a doctor said it was impossible. Not because you did any research. Because it seemed obvious. Of course that is over now. Of course HIV changed that.
Here’s what we want you to know: that assumption was wrong. And the fact that nobody corrected it, that your doctor probably never brought it up, that the information never found you, that is not your fault. That is a gap in the system.
And we’re here to close it.

The Answer Is Yes
HIV+ gay men can become biological fathers. Not despite modern medicine, BUT because of it.
HIV status is far less of a barrier than most men have been led to believe. Science moved forward years ago. The conversation just didn’t follow. There are multiple safe, well-documented pathways to biological fatherhood available to you right now, and we’ll walk through each of them plainly and honestly in this article.
But before we get to the how, we need to talk about something more important: why so many men never even got to ask the question.
Three Safe Pathways to Biological Fatherhood
Once you understand the science, the practical pathways become much clearer. Here are the three main routes, explained without medical jargon, without minimizing the journey, and without leaving anything important out.

Pathway 1: U=U – With a Confirmed Undetectable Viral Load
You’ve probably heard the term U=U. Now, there’s a good chance nobody has ever connected it to fatherhood.
But this connection is the heart of this article.
U=U stands for Undetectable = Untransmittable.
It is one of the most significant developments in HIV medicine in decades, and since it was officially endorsed by major health organizations worldwide in 2017, it has fundamentally changed what it means to live with HIV.
In plain language: when a person living with HIV is on antiretroviral therapy (ART) and maintains a consistently undetectable viral load, they cannot transmit HIV to another person. Not to a sexual partner. Not to a surrogate. Not to a child.
If you are undetectable, you are not a transmission risk. Full stop.
For many HIV+ gay men, the dream of fatherhood wasn’t taken away by biology. It was taken away by a story. A story that said HIV means danger, infection, closed doors. U=U rewrites that story. It doesn’t just protect others from transmission. It gives you back your future.
Let’s check out the research, published in BMC Public Health by Dr. Robert Pralat and colleagues at University College London. They found that most HIV+ gay men had never discussed fatherhood with their healthcare provider at all. Of 25 men interviewed, half of whom wanted children, only four had ever had that conversation in a clinical setting. The men weren’t avoiding the topic. The doctors just weren’t asking.
As the researchers concluded: “Contrary to what clinician commonly assumed, many men expressed interest in receiving more information, highlighting the importance of reassuring people upon diagnosis that it is possible to become parents while living with HIV.”
Fatherhood and longevity. Hope and the future.
These things are bound together in ways that go deeper than any medical chart.
Pathway 2: Sperm Washing + IVF or IUI
“It might even have been [when I was diagnosed]. I know someone mentioned, don’t worry, you can still have children, there’s this thing called sperm washing.Someone at least mentioned just about everything I may have had an issue with, so I was at least aware. And then they brought it up again at the [HIV support] group. So I knew it was an option. (William, aged 28).”
You may have heard of sperm washing in passing – something a friend mentioned, something you stumbled across online. For many men, it exists vaguely in the imagination as something complicated, clinical, and perhaps experimental.
Here is what it actually is: a laboratory process in which sperm is separated from seminal fluid. Since HIV lives in the seminal fluid and not in the sperm cells themselves, this separation removes the virus from the equation entirely. The washed sperm is then used for IVF (in vitro fertilization) or IUI (intrauterine insemination) with a surrogate or egg donor.
Read more on this topic in our blog post How to Do IVF with Donor Eggs: A Complete Beginner’s Guide
The safety record is extraordinary. A 2016 meta-analysis published in the journal Fertil Steril reviewed 40 studies and found zero cases of HIV transmission across 11,585 sperm washing procedures involving almost 4,000 women. Zero. Not a single documented transmission.
One fear we hear often: will any surrogate agree to carry for an HIV+ intended father? This fear is real and understandable. And it is also not the reality. Most surrogates, when properly and fully informed about sperm washing and U=U, say yes.
Pathway 3: Layered Protection – U=U + Sperm Washing + PrEP
Some men, agencies, and surrogates prefer to use multiple layers of protection together, not because any single layer is insufficient, but because stacking them provides a level of certainty that removes doubt entirely.
The combination works like this: the intended father maintains an undetectable viral load (U=U), the sperm is washed in the lab before use, and the surrogate takes PrEP (pre-exposure prophylaxis) as an additional shield. With all three in place, the transmission risk is essentially theoretical. It exists only on paper.
There is no requirement to use all three. But for men who have carried this fear for a long time, who need to feel completely certain before they open this door, this combination exists, it works, and it is available.
The Question That is Stealing Your Sleep: Do I Qualify?
Before diving into pathways and programs, there’s a practical question worth answering directly: what do you actually need to have in place before any of this becomes available to you?
The good news is that the bar is achievable, and for many men already managing their HIV well, it may be closer than they think.
Here is what fertility clinics and surrogacy programs typically require of HIV+ intended fathers:
- An undetectable viral load, sustained for at least six months.
This is the non-negotiable foundation. Most programs require documentation showing that your viral load has been fully suppressed, generally below 48–50 copies per milliliter, for a minimum of six consecutive months before you begin the process. This isn’t a bureaucratic hurdle. It’s the scientific basis for everything that follows.
- Consistent adherence to antiretroviral therapy (ART).
Programs want to see that your viral suppression is stable and maintained, not a one-time result. This means being on ART, taking it as prescribed, and being regularly monitored by your HIV care team.
- STI screening.
A standard panel for sexually transmitted infections is required before proceeding. This is routine for all intended parents, not specific to HIV+ individuals.
- Semen testing.
Not just blood testing. This one surprises many men, and it’s worth understanding clearly. HIV viral load in your blood and HIV viral load in your semen are not always the same thing. A man can have an undetectable blood viral load and still have detectable virus in his seminal fluid, because the organs that produce semen can harbor HIV independently of what shows up in a blood test. This is precisely why programs like SPAR at the Bedford Research Foundation test semen directly, using a highly sensitive PCR HIV DNA assay, rather than relying on blood results alone. Semen samples that test positive are discarded. Only samples confirmed to be virus-free proceed.
If you’re not yet at the undetectable stage, or if you’re newly diagnosed and still finding the right medication regimen, this is not a closed door. It is a timeline. Many men have used the months of working toward consistent viral suppression as the same months they used to research, plan, and prepare. The journey can begin before the eligibility box is fully checked.
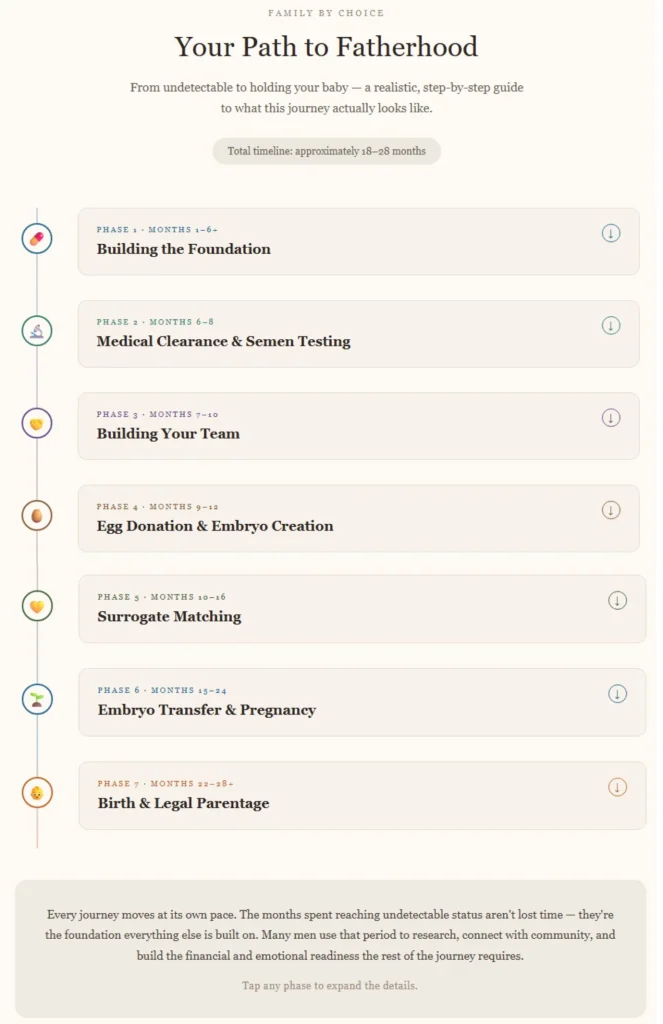
What Happens on Both Sides: The Surrogate’s Protection
This is the question many HIV+ intended fathers carry quietly: what exactly am I asking her to do?
It’s worth answering directly, not just to reassure you, but because understanding the protections in place for your surrogate is what transforms abstract confidence into something real.
From your side as the intended father:
If you checked the timeline we placed in an infographic, above, you already know that, before any surrogate is ever involved, the medical work is already done. Your viral load is confirmed undetectable. Your semen has been tested directly, not just your blood, using a PCR HIV DNA assay at SPAR or an equivalent program. Any sample containing detectable virus has been discarded. The sperm used for fertilisation has been washed and confirmed virus-free. By the time an embryo exists, it has been created from material that has passed multiple layers of screening. Your gestational surrogate is never exposed to your semen. She receives an embryo.

From her side:
Your surrogate is told everything. Your HIV status, what sperm washing is, how SPAR works, what the science shows, and what the real-world transmission record looks like. This is not disclosed in fine print. Informed consent is a formal, documented part of the process. She is given the opportunity to ask questions, speak with a medical professional, and consult with her primary support person, who must also be on board. She chooses to proceed freely, with full information, not in spite of the risks but because she understands there aren’t meaningful ones.
Since this is gestational surrogacy, before the embryo transfer, she may be offered PrEP, as an additional precautionary measure. This is a well-established HIV prevention medication that has been safely used during early pregnancy.
After the transfer, she receives HIV antibody testing at three weeks, three months, and six months. This monitoring is standard protocol in HIV+ surrogacy programs. It is not because transmission is expected, because across thousands of procedures it has never occurred, but because her health is taken seriously at every stage, not just before the process begins.
What this means for you:
You are not asking your surrogate to take a risk and hope for the best. You are entering a process that has been specifically designed, tested, and refined to protect her, with multiple independent safeguards, mandatory disclosure, genuine consent, preventative medication, and ongoing monitoring.
The surrogates who participate in these programs know exactly what they are doing. Many actively seek to work with HIV+ intended parents. That isn’t naivety. It’s an informed decision made by women who have looked at the same evidence you’re reading now and reached the same conclusion: the science is sound, the protections are real, and the family on the other side of this is worth showing up for.
The Myth That Quietly Stole Fatherhood From Too Many Men
One man described the moment he was diagnosed and what he assumed it meant for his future. His words stayed with us:
““[If] they told me, ‘Listen, you’ll have boyfriends, you’ll be fine…. But at that point, you can’t really hear that,” he said. “The idea of having kids…just in a practical sense, like, well, this cannot happen. You know, my sperm is now sullied, it cannot be used by anyone.”
He is not alone in believing this. Across multiple studies, HIV+ gay men consistently described their sperm as infected, unusable, or dangerous, a belief so deeply held that many never sought medical advice to the contrary. They closed the door themselves, before anyone pushed them.
We want to say this as directly and gently as we can:
HIV does not live in sperm cells. It lives in seminal fluid, the liquid surrounding sperm. The sperm themselves are healthy.
This is not a technicality. This is the scientific foundation of everything in this article. The sperm that could give life to your child is not infected. It has always been healthy. This is exactly why sperm washing works, it separates the healthy sperm from the fluid that carries the virus. And this is exactly why U=U applies to reproduction, when the virus is undetectable, it cannot be passed on through any route.
Your body’s ability to father a child was not taken from you at diagnosis. The door was always open. It just wasn’t shown to you.
What Getting Started Actually Looks Like
You don’t need to have everything figured out before you take a first step. The first step is simply getting informed and finding the right people to talk to.
Medically, here is where to begin. Make sure you are on ART and consistently undetectable. This is the foundation of every pathway. Consider a semen analysis, because HIV+ men can sometimes have fertility factors worth knowing before choosing a route forward. Find an HIV-affirming fertility specialist or reproductive endocrinologist. Not all fertility clinics have experience with HIV+ patients, so look for clinics that explicitly welcome HIV+ intended parents.
Ask about sperm washing availability. Some clinics offer it in-house, others refer to specialized programs like SPAR at the Bedford Research Foundation. If surrogacy is on your mind, look for agencies with explicit HIV-inclusive programs; Circle Surrogacy has been working with HIV+ gay men since 2009.
Emotionally, know this: this journey can bring up things you didn’t expect. The grief of having carried a false belief for years. The relief of learning it wasn’t true. The strange, complicated mix of hope and fear that comes with opening a door you thought was permanently closed.
You are allowed to feel all of it. And you don’t have to navigate it alone. Research consistently shows that HIV+ men who connect with others who have walked this path, who felt the same fears, asked the same questions, and came out the other side as fathers, build a confidence that no medical pamphlet can provide.
Community isn’t a luxury in this journey. It’s part of how you get there.
The Door Was Never Closed
The science is clear. HIV+ gay men can become biological fathers through multiple safe, well-documented pathways. U=U means an undetectable viral load effectively eliminates transmission risk. Sperm washing has a perfect safety record across tens of thousands of procedures. Programs, agencies, and clinics exist specifically to support you through this.

But beyond the science, here is what we most want you to take away:
The dream of fatherhood that you quietly set aside when you were diagnosed? It belongs to you. It was always yours. HIV did not take it.
The gap between what medicine knows and what you were told is not a reflection of what is possible for you. It is a reflection of a system that hasn’t caught up with the men it serves.
You deserve a provider who asks the question. You deserve clear, honest, empowering information. Not fear, not outdated assumptions, and not silence. And you deserve a community that understands what this journey actually feels like.
That is what Family By Choice is here for.
Ready to take the next step?
Our LGBTQ+ Family Building and Surrogacy Journey courses are taught by fertility specialists, surrogacy consultants, and legal experts who understand your path. If you’re an HIV+ gay man exploring fatherhood, or just beginning to let yourself consider it, these courses were built with you in mind.
Explore all LGBTQ+ and surrogacy courses
Want access to everything?
Family By Choice membership gives you unlimited access to our full course library – including LGBTQ+ family building, surrogacy, donor conception, mind and body preparation, and live Q&A sessions with experts. A community of people who get it is waiting for you.
Check out our membership options

