Deciding between conventional IVF insemination and intracytoplasmic sperm injection (ICSI) can be overwhelming for future parents. Both are methods of fertilizing eggs in the IVF lab, but they differ in technique and when they’re needed.
It’s normal to feel unsure about which is best for your situation. After all, you want the highest chance of success while minimizing costs and risks.
In this article, we’ll explain what each method involves, their benefits and limits, and which scenarios each is suited for.
We’ll also discuss costs (and whether insurance covers ICSI), success rates, and when not to use one method or the other.
Our aim is to give you honest, evidence-based information so you can feel informed and supported in your fertility journey.
Remember, every couple’s case is unique, and your fertility specialist will help guide you – but understanding the basics can make those decisions a bit less stressful.
What Is Conventional IVF Insemination
Conventional IVF insemination is the classic method of fertilization used in IVF. In this approach, a prepared semen sample (containing thousands of sperm) is added to the dish containing the retrieved eggs and then nature takes its course. The sperm must swim and penetrate the egg on their own without direct assistance.
Typically, each egg is placed in a lab dish with ~50,000 to 100,000 moving sperm, mimicking the natural fertilization process (just outside the body). Only one sperm should ultimately burrow into and fertilize each egg, forming an embryo.
Fertilization is usually checked the next day to see how many eggs became fertilized embryos.
This method has been used since the earliest days of IVF (the first IVF baby was born in 1978). It relies on having a sufficient quantity of healthy, motile sperm. If the sperm parameters are within normal ranges, conventional insemination often works well. Approximately 70% of mature eggs fertilize on average in a typical IVF cycle, though rates can vary based on egg/sperm quality and fertilization method used.
Importantly, conventional IVF lets the sperm compete naturally to fertilize the egg, which means the “best” sperm (the one that is able to bind to and penetrate the egg) will win out as it would in natural conception. Many couples find comfort in this more “natural” fertilization process, since it involves less manipulation of the gametes.
However, conventional IVF does not guarantee that fertilization will happen – there is a small risk that none of the eggs will fertilize if the sperm are unable to penetrate them. In fact, if sperm count or motility is too low, there is a high chance that fertilization may fail entirely with conventional IVF. For this reason, conventional insemination is usually only attempted when the sperm analysis is fairly normal and there’s no known severe male-factor infertility.
We’ll discuss later what limits this method has and when it might not be suitable. First, let’s define ICSI, the alternative fertilization method.
What Is ICSI (What Is Intra-Cytoplasmic Sperm Injection)
ICSI (intracytoplasmic sperm injection) is a specialized lab technique introduced in 1992 to help fertilize eggs, particularly for cases of male infertility. In ICSI, instead of leaving sperm to swim to the egg on their own, an embryologist selects a single sperm and injects it directly into the cytoplasm of the egg using a microscopic needle.
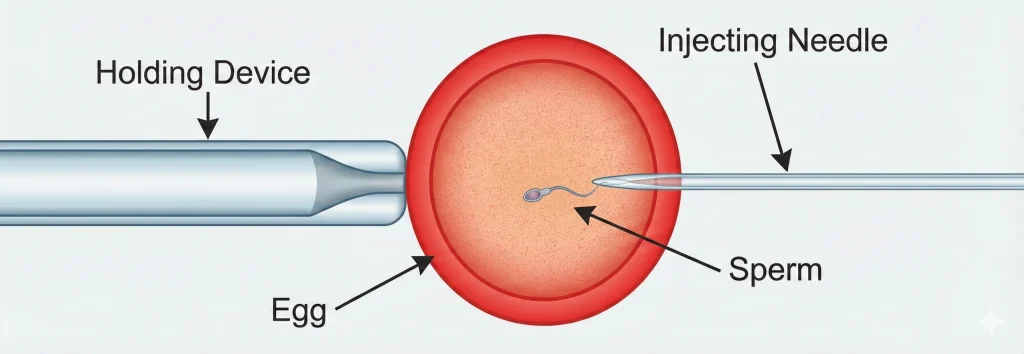
Diagram illustrating the ICSI process. A single sperm is picked up in a fine needle and injected into the egg, enabling fertilization even when sperm cannot penetrate the egg on their own.
ICSI bypasses the usual hurdles a sperm has to overcome (swimming to the egg, attaching to and penetrating the egg’s outer layer). This method was revolutionary because before ICSI existed, men with very poor sperm quality often had to resort to donor sperm. ICSI offered hope that these men could still father their own genetic children.
It’s important to note that ICSI is actually an addition to IVF, not a completely separate treatment. The overall IVF process (ovarian stimulation, egg retrieval, embryo culture, etc.) is the same as conventional IVF for the patient. The onlydifference is how the eggs get fertilized in the lab.
With ICSI, the lab procedure is more hands-on: each mature egg is individually injected with a sperm. Because of this, ICSI requires highly skilled embryologists and special micromanipulation equipment. In ICSI, only mature eggs are injected, and published studies typically report fertilization rates for injected eggs in a range of roughly 50–80% depending on patient and laboratory factors.
What are the benefits of Conventional IVF Insemination?
Conventional IVF insemination offers several advantages in appropriate situations (mainly when sperm parameters are normal). Key benefits include:
- Less Invasive Fertilization: The egg and sperm meet in a dish and fertilize “naturally,” without a needle penetrating the egg. This avoids the physical manipulation of the egg that ICSI entails, eliminating any direct injection-related risk to the egg. There’s no handling of each egg under a microscope, which some couples find more reassuring.
- Natural Sperm Selection: Because many sperm are competing to fertilize the egg, typically only a healthy, capable sperm can succeed in entering the egg on its own. This means conventional IVF allows a form of natural selection – the fastest or most competent sperm gets in.
- Avoids Unnecessary Procedures: If there’s no indication for ICSI, sticking with conventional insemination means one less procedure in the lab. ICSI adds extra steps (and cost), so if it’s not needed, skipping it keeps the IVF process simpler and cheaper.
- Lower Cost: Conventional IVF is less labor-intensive, so it doesn’t carry the extra fee that ICSI does. We’ll detail the cost later, but broadly, opting for conventional insemination can save you a significant amount of money in your IVF cycle if ICSI isn’t truly necessary.
So, when the male partner’s sperm count, motility, and morphology are adequate, conventional IVF is usually very effective. It has the advantage of being closer to natural fertilization and avoids the additional procedures and costs of ICSI. So if your doctor tells you your sperm looks good, it’s possible that conventional insemination will be suggested.
What are the benefits of ICSI (Intra-Cytoplasmic Sperm Injection)?
ICSI comes with several important benefits, especially for certain fertility challenges. The main advantages of ICSI include:
- Overcoming Severe Male Infertility: This is the original and biggest benefit. ICSI allows fertilization even when sperm count or motility is extremely low, or other sperm problems exist that would prevent natural fertilization. By injecting a single sperm into an egg, ICSI bypasses issues like poor swimming ability or inability to penetrate the egg. Men who previously would have had no chance of fertilizing an egg (e.g. men with only a few viable sperm, or sperm retrieved surgically from the testes) can achieve fertilization through ICSI.
- Avoiding Complete Fertilization Failure: Even outside of obvious male-factor cases, ICSI is often used as an “insurance policy” against the heartbreaking scenario of getting zero fertilized eggs. In some couples (e.g. with unexplained infertility or borderline sperm parameters), there might be hidden sperm–egg interaction issues. ICSI greatly reduces the risk of total fertilization failure, because each egg gets a sperm injected directly. So, logically, when ICSI is used, the odds of having no fertilized eggs at all are lower than with conventional insemination.
- Enables Use of Sperm Collected by Surgical Retrieval: If sperm must be obtained through procedures like PESA or TESE (where sperm are taken from the epididymis or testicle due to blocked ducts or other issues), it’s possible that ICSI will be suggested first. Such sperm often are few in number or not mature enough to move and penetrate an egg on their own. ICSI makes it possible to fertilize eggs with these surgically retrieved sperm, whereas conventional IVF with these samples might not succeed.
- Useful for Certain Lab Situations: There are a few specific scenarios where ICSI offers practical benefits:
- Preimplantation Genetic Testing (PGT): When doing genetic testing on embryos, some clinics prefer to use ICSI. The reason is that with conventional insemination, multiple sperm can stick to the outside of the egg, and their DNA could contaminate the genetic testing of the embryo. Using ICSI (injecting a single sperm and washing away extras) avoids that contamination risk. So if you plan to do PGT for embryo screening, ICSI might be recommended to ensure accurate results.
- Fertilizing Previously Frozen Eggs: Eggs that have been cryopreserved (vitrified and thawed) tend to have a hardened zona pellucida (outer shell), making it harder for sperm to penetrate naturally. ICSI is commonly used with frozen eggs to achieve good fertilization rates. Some egg banks and programs mandate ICSI for thawed donor eggs.
- Prior IVF Fertilization Failure: If a couple had an earlier IVF cycle where conventional insemination yielded very poor or no fertilization, adding ICSI in the next attempt can improve outcomes.
- Preimplantation Genetic Testing (PGT): When doing genetic testing on embryos, some clinics prefer to use ICSI. The reason is that with conventional insemination, multiple sperm can stick to the outside of the egg, and their DNA could contaminate the genetic testing of the embryo. Using ICSI (injecting a single sperm and washing away extras) avoids that contamination risk. So if you plan to do PGT for embryo screening, ICSI might be recommended to ensure accurate results.
- High Fertilization Rates per Egg: When conditions are right, ICSI fertilizes a fair proportion of eggs. Since the lab has a goal to provide each egg with a sperm, you might be less likely to “waste” eggs. So ICSI as a procedure has a goal to maximize the number of embryos you get from a given batch of eggs, which can be useful if egg supply is limited.
Overall, ICSI’s biggest advantage is that it opens the door to IVF success for couples who would otherwise have little to no chance with conventional fertilization. It gives amazing results in cases of fertilization problems affected by severe male infertility, and it can provide a “safety net” against fertilization failure in “tricky” situations. Thanks to ICSI, thousands of men with issues like some kinds of azoospermia (no sperm count) or very poor sperm quality have been able to biologically father children.

What are the limits of Conventional IVF Insemination?
While conventional IVF might be more effective to some, we must be aware that it also has limitations and drawbacks, particularly in cases involving male infertility. The main limits of conventional insemination include:
- Requires Sufficient Quantity & Quality of Sperm: Conventional IVF won’t work well if the sperm sample is severely impaired. There is a threshold of sperm count and motility needed to reliably fertilize eggs in a dish. If a man’s sperm count is very low (oligospermia) or the sperm have poor motility, the chance that any sperm will make it into an egg is not so great. For instance, with a count of only a few thousand sperm, an egg in a dish might never encounter a viable sperm at all. In such cases, conventional IVF could lead to zero embryos. Thus, a significant limitation is that couples with moderate to severe male factor infertilityare not good candidates for conventional insemination – it simply may not achieve fertilization.
- Risk of Total Fertilization Failure: Even in couples without obvious sperm issues, conventional IVF carries a small risk that none of the eggs fertilize. Studies have shown that 5–10% of IVF cycles using conventional insemination can end up with total fertilization failure (no embryos). This can happen due to subtle sperm–egg interaction problems or egg quality issues that aren’t apparent beforehand. That kind of outcome is devastating after all the effort of an IVF cycle.
- Not Suitable for Certain Special Cases: As mentioned earlier, conventional insemination generally is usually not used if sperm are obtained surgically from the testis/epididymis, or if you are fertilizing thawed eggs. Also, if you need PGT on embryos, conventional IVF is not ideal because stray sperm on the egg can interfere with embryo DNA testing. In these cases, the limitation of conventional IVF is that it might force a compromise on outcomes or lab procedures. Therefore, in some clinics conventional IVF is essentially “off the table” for those situations – ICSI will be used instead.
- Possible Lower Fertilization Rate per Egg (in some contexts): While conventional IVF often fertilizes a good proportion of eggs, the fertilization rate can be lower compared to ICSI. For example, if there are subtle issues with sperm binding to the egg, you might see only, say, 40–50% of eggs fertilize conventionally when ICSI could have fertilized 60–70%. This means potentially fewer embryos to work with. If only a few eggs are retrieved to begin with, losing any due to fertilization failure is a significant limitation.
What are the limits of ICSI (Intra-Cytoplasmic Sperm Injection)?
ICSI is a powerful technique, but it also has its limitations and downsides to consider. Some of the key concerns and limitations of ICSI include:
- Additional Cost and Resources: ICSI adds a significant cost to an IVF cycle because it’s labor-intensive. An embryologist must inject each egg individually, using costly precision equipment. This typically incurs an extra fee. For couples paying out of pocket, this could be a non-trivial limitation. It also can use more laboratory time and expertise, which is why many clinics charge separately for it.
- Invasiveness & Egg Damage Risk: Unlike conventional IVF, ICSI involves physically penetrating the egg with a needle. This procedure, while routine, is not without risk – a small percentage of eggs can be damaged or destroyed by the injection process. Even in the hands of experienced embryologists, some eggs (usually a few percent) may not survive ICSI due to the trauma. Additionally, only mature eggs can tolerate injection; any eggs that aren’t mature at the time cannot be fertilized at all with ICSI, which could be seen as a limitation (though this is also true for conventional IVF – immature eggs won’t fertilize naturally either).
- Bypassing Natural Sperm Selection: ICSI circumvents the natural filters that typically let only the healthiest sperm fertilize an egg. In ICSI, the lab technician selects a sperm based on appearance and motility, but they cannot assess its DNA integrity or other hidden defects just by looking. This means a sperm that would have lost the race in natural fertilization (perhaps due to subtle abnormalities) might still end up fertilizing the egg via ICSI. The concern here is that ICSI could potentially increase certain risks if an abnormal sperm (one that would normally not fertilize an egg) is inadvertently used.
- Potential (Small) Increase in Genetic or Developmental Risks: Because ICSI is relatively new in the scope of human reproduction (first babies born in 1992), researchers have been carefully tracking outcomes. The good news is that so far, children born from ICSI appear just as healthy as those from conventional IVF. However, ICSI might carry a slightly higher chance of certain genetic or epigenetic issues, simply because it bypasses some natural checks and often involves parents with fertility issues.
- No Improvement in Outcome if Not Needed: One could frame this as a limitation – if the male partner’s sperm is normal, ICSI doesn’t typically boost pregnancy success rates compared to conventional IVF. So an inherent “drawback” of ICSI is that doing it when it’s not indicated doesn’t help you get pregnant faster, it just costs more and exposes you to the small risks mentioned above. Fertility specialists criticize the overuse of ICSI for this reason: it’s an amazing tool when needed, but using it on everyone isn’t beneficial on a population level.
Which Patients Benefit From Which Approach
Now that we’ve covered pros and cons, which type of patient is suited for conventional IVF vs. ICSI? In practice, fertility doctors will recommend one method or the other based on the couple’s specific diagnosis and history.
Patients who benefit from Conventional IVF (no ICSI needed):
- Couples with Normal Sperm Parameters: If the male partner’s semen analysis shows a normal or only mildly suboptimal sperm count, motility, and morphology, conventional insemination might be the first-line approach. These couples have a high likelihood of fertilization without needing ICSI. Using conventional IVF avoids unnecessary cost and intervention in this scenario.
- Unexplained Infertility (with normal sperm tests): Many couples with unexplained infertility (no obvious male or female factor) will usually start with conventional IVF. Unless there’s a suspicion of a fertilization problem, conventional insemination will most likely be suggested. So if sperm is fine, these patients can benefit from trying conventional, knowing ICSI is a backup if something goes wrong.
- Women with Plenty of Eggs (buffer against failure): If a patient has a good ovarian response and many eggs retrieved, doctors might be comfortable doing conventional IVF because even if a slightly lower fraction fertilize, there will still be enough embryos. Essentially, if you have a lot of eggs and normal sperm, the risk of total fertilization failure might be low (because it rarely happens that all eggs fail to fertilize if sperm are fine). Thus, patients with robust egg numbers can benefit from conventional IVF without ICSI, knowing they have a cushion.
- Cost-Sensitive Patients (without male factor): For those paying out of pocket or with limited insurance, and who do not have male infertility, sticking with conventional IVF can be a financially less burdening. They can allocate those funds to other needs or another cycle if needed.
Patients who benefit from ICSI:
- Male Factor Infertility: Any couple where the male partner has significantly abnormal semen parameters will almost certainly be steered toward ICSI. This includes very low sperm count, very poor motility, or severe teratozoospermia (very few normal-shaped sperm). It also includes some kinds of cases of azoospermia (no sperm in ejaculate) where sperm are obtained surgically. In these conditions, ICSI is often the suggested procedure to achieve fertilization – conventional IVF could lead to a high failure rate or be impossible. Patients with these issues clearly benefit from ICSI’s ability to use even rare or weak sperm to create embryos.
- Prior Fertilization Failure or Low Fertilization: Couples who went through a conventional IVF cycle that resulted in zero fertilized eggs (or an unexpectedly low fertilization rate) are also candidates for ICSI in the next attempt. There may be anti-sperm antibodies or other hidden factors at play. Using ICSI could solve that problem in the subsequent cycle. Even one prior failed fertilization is usually enough for doctors to recommend “doing ICSI this time” to avoid repeating the disappointment. These patients benefit because ICSI can literally salvage a situation where conventional IVF did not work before.
- Limited Egg Supply: If a patient has only a few eggs to work with (for example, poor responders or older patients retrieving very low egg numbers), some clinics will suggest ICSI. The reasoning is that with, say, only 2 or 3 eggs, you really want to make sure each one has the best chance to fertilize. The couple might not want to risk losing all of them to a fertilization issue. In this sense, patients with a limited number of eggs may benefit from ICSI as a precaution to maximize the odds that each precious egg becomes an embryo.
- Use of Advanced Lab Procedures: Patients planning to use preimplantation genetic testing (PGT) on their embryos, or those using frozen eggs or certain other lab techniques, often benefit from ICSI. As mentioned earlier, ICSI is generally recommended for PGT cases to avoid DNA contamination. So if you fall into that group (say you’re doing IVF to test embryos for a genetic disease or for aneuploidy screening), ICSI would be the method of choice. Likewise, if you’re using donor eggs that were frozen, or your own previously frozen eggs, most clinics will use ICSI to fertilize them. Patients in these categories benefit because ICSI is effectively part of the standard protocol to ensure those processes work optimally.

What is the cost difference between conventional IVF and ICSI?
One practical consideration is cost. ICSI is an add-on laboratory procedure, and it does cost extra compared to conventional IVF. The exact cost difference varies by clinic and country, but generally:
- ICSI carries an extra fee: Most fertility clinics charge a separate ICSI fee on top of the base IVF cost. This fee accounts for the additional lab work and equipment. In many cases, ICSI costs roughly 20–30% more than standard IVF.
By contrast, conventional IVF insemination has no such extra fee, because the embryologist simply combines sperm and eggs in a dish and lets them incubate, a procedure that takes far less hands-on time. So from a cost perspective, there’s a clear difference: ICSI makes your IVF cycle pricier.
Of course, the value of that extra cost depends on your situation. For some couples, it’s absolutely worth it because without ICSI they might not get any embryos at all (so the extra cost might lead to a better chance of success). For others, it may be an unnecessary expense if their odds of fertilization were fine without it.
Cost is an important discussion to have with your clinic’s financial counselor: ensure you know how much ICSI would add and under what conditions it’s recommended or optional.
Which method gives better embryo development?
A common question is whether embryos created via conventional fertilization are “better” or “worse” than those created via ICSI. In terms of embryo development and quality, the consensus from research is that there is a slight difference in embryo quality between the two methods when used appropriately.
In summary, neither method universally creates “better” embryos. If anything, what matters is using the right method for the right couple: that maximizes the chance of getting any good embryos. When ICSI is indicated and used, it gives you embryos that you wouldn’t have had otherwise (which is a clear win). When it’s not indicated, using it doesn’t improve embryo quality, and not using it doesn’t harm embryo quality. So you can rest assured that a baby conceived via conventional IVF or via ICSI has passed through similar embryo development milestones in the lab. The key is getting to those embryos in the first place by choosing the appropriate fertilization method for your situation.
Does insurance cover ICSI, or is it an extra charge?
Health insurance coverage for fertility treatments is highly variable globally, but ICSI is often considered an “extra” (add-on) service rather than a standard inclusion. In many cases, insurance will cover the basic IVF procedure (if you have infertility coverage at all) but may not automatically cover ICSI unless certain criteria are met.
Is ICSI worth the extra cost if we don’t have male factor infertility?
This is a very common question from patients who technically could fertilize their eggs with conventional IVF. The honest answer, based on current evidence, is: Usually, no – if you don’t have male factor issues, ICSI is not likely to increase your chance of success.
Here’s why:
- No clear success rate improvement: Extensive research has compared IVF vs. ICSI in couples without male infertility, and they’ve found no significant improvement in pregnancy or live birth rates by doing ICSI. The evidence suggests that if the chance of live birth following c-IVF is assumed to be 32%, the chance of live birth with ICSI would be between 30% and 41%.
“The current available studies that compare ICSI and c-IVF in couples with males presenting with normal total sperm count and motility, show neither method was superior to the other, in achieving live birth, adverse events (multiple pregnancy, ectopic pregnancy, pre-eclampsia and prematurity), also alongside secondary outcomes, clinical pregnancy, viable intrauterine pregnancy or miscarriage.” (source) - When might it be worth it? The main potential benefit for a non-male-factor couple is the reduction in risk of total fertilization failure. If you have a very low tolerance for that risk (even if it’s small), you might consider ICSI for peace of mind. For instance, say a couple has unexplained infertility and retrieved only 3 eggs – they might choose ICSI despite normal sperm, just to avoid the possibility that none of those 3 fertilize.
- Consider the cost-benefit: If money is a concern, and there’s no strong indication for ICSI, then skipping ICSI can be a reasonable way to save on your IVF cycle.
- Professional guidelines: Professional fertility guidelines emphasize that routine use of ICSI in patients who don’t need it is not recommended. They encourage doctors and patients to use ICSI judiciously – basically, only when it’s likely to make a difference. So if you have normal sperm and no other indication, most experts would say ICSI is not worth it purely as a blanket add-on, because it adds cost and slight procedural risk without boosting success. That being said, patient preference matters too. If a patient understands the evidence and still feels more comfortable doing ICSI “just in case,” some clinics will accommodate that choice (especially if the patient is paying and wants that reassurance).
When NOT to Use ICSI
ICSI is a wonderful tool, but there are scenarios where it is not recommended to use ICSI (i.e. you should not do ICSI). Broadly, you should not use ICSI when there is no clear benefit to using it. Concretely:
- Routine use in normal cases is discouraged: If the male partner’s sperm is normal and there’s no history of fertilization failure, ICSI is generally not advised.
- When it contradicts a patient’s values or circumstances: Some patients may have ethical or personal reasons to avoid ICSI (for example, discomfort with the idea of micromanipulation of gametes). While this is less common, if a patient strongly prefers not to bypass natural fertilization and there is no medical necessity for ICSI, then ICSI should not be forced.
- If using donor sperm with excellent quality: Typically donor sperm is of very high quality. In IVF cycles with donor sperm (and a healthy egg provider), ICSI is often unnecessary.
Basically, do not use ICSI without a reason. Every medical intervention should have a rationale. So you don’t use ICSI when the only rationale would be convenience or habit. Even though many clinics have gotten into the habit of doing ICSI almost routinely, best practices say not to do that unless indicated. The potential downsides (cost, slight risks) don’t justify it in low-risk scenarios.
When Not to Use Conventional IVF Insemination?
Conversely, there are situations where you should not use conventional IVF insemination because it would likely fail or be suboptimal. In such cases, ICSI is the clear choice. You would avoid conventional fertilization when:
- Severe Male Factor Infertility: If the sperm parameters are well below normal thresholds (for example: extremely low count, near-zero motility, or virtually no normal forms), you should not attempt conventional IVF.
- Obstructive or Non-obstructive Azoospermia (sperm retrieved surgically): If the man has no sperm in the ejaculate and sperm are obtained via procedures like TESE or PESA, conventional IVF is not an option. Those sperm often come in very low numbers and/or are not able to swim properly, so you cannot use conventional insemination with surgically retrieved sperm.
- History of Fertilization Failure: If a previous IVF cycle with conventional insemination resulted in little to no fertilization, you would not try conventional again the next time. As NICE guidelines put it, ICSI should be considered if a prior IVF cycle had failed or very poor fertilization.
- Egg-Related Situations: If you have circumstances like using thawed eggs or doing something like in vitro maturation (IVM) of eggs, conventional insemination is often not recommended. Many clinics simply will not do conventional fertilization on previously frozen eggs because the success would be limited – they go straight to ICSI. Similarly, for IVM (a more experimental scenario where eggs are matured in the lab), ICSI is usually used because those eggs might not fertilize easily on their own. Therefore, do not rely on conventional fertilization for eggs that have special circumstances (like having been frozen or otherwise manipulated).
- Preimplantation Genetic Testing cases: As mentioned, if PGT is part of the plan, most labs will not use conventional insemination due to the contamination issue. So one would not use conventional IVF in a PGT-M (monogenic disease) case, for example, because leftover sperm DNA could complicate the genetic test. In practice, conventional IVF is not used when high-precision genetic testing is needed on embryos.
Navigating the decision of conventional IVF vs. ICSI can be daunting, but it all comes down to understanding your own fertility diagnosis.
If you’re dealing with male factor infertility or other specific hurdles, ICSI can be a game-changer that opens the door to pregnancy. If not, you can take comfort that conventional IVF is usually just as effective without extra cost or complexity.
Always have a thorough discussion with your fertility doctor about why they recommend one approach for you.
The goal is the same in both cases – a healthy embryo and a healthy baby – and by using the method best suited to you, you maximize your chances of making that dream a reality.
Good luck, and remember that whatever method is used, the success of IVF ultimately rests on factors that you’re working on improving (like egg quality, sperm health, and uterine receptivity). Stay hopeful and informed, and lean on your medical team for guidance as you make these decisions.


